How to Survive Night Shift Nursing: A Nurse’s Complete Guide
TL;DR: Cluster your night shifts and maintain your sleep schedule on days off to reduce circadian chaos. Set a hard caffeine cutoff 4 to 6 hours before you plan to sleep. Eat low-glycemic meals during your shift to avoid energy crashes at the worst moments. Tackle high-focus tasks before 2 AM. Use the 3 AM…

Surviving night shift nursing comes down to three things: protecting your sleep, managing your body’s circadian biology, and building systems that hold up across a 12-hour shift. This guide covers every layer of how to survive night shift nursing: your first week on nights, the 3 AM wall, caffeine strategy, and long-term sustainability.
Is Night Shift Nursing Hard to Adjust To?
Yes, and the difficulty is physiological, not a matter of willpower. Your body’s circadian rhythm is governed by light cues that promote wakefulness during the day and sleep at night. Night shift work forces you to fight that biology directly. A Cureus review (2025) examining 74 studies found that night shift nurses consistently show reduced alertness, impaired cognitive performance, and disrupted sleep compared to day shift counterparts.
The good news: nurses who learn how to survive night shift nursing through deliberate habits around sleep, nutrition, and schedule management adapt faster and sustain performance better than those who improvise. This guide gives you those habits.
What Should You Do in Your First Week on Night Shift?
Your first week sets the baseline for everything that follows. The adjustments you make now determine how hard the next month feels.
Before your first shift:
- Stay up late the two nights before your first night shift. Aim for a 2 to 3 AM bedtime to begin shifting your circadian window earlier.
- Take a 20 to 30 minute nap in the late afternoon before your first shift. Research on healthcare shift workers shows that pre-shift napping meaningfully reduces sleepiness during the first night, which is typically the hardest.
- Get your blackout curtains, eye mask, and phone silencer set up before you need them.
Scheduling strategy:
Request clustered shifts if your unit allows it. Working two or three nights in a row is harder in the short term but far easier on your circadian rhythm than alternating nights. Each time you flip back to a daytime schedule, you essentially give yourself jet lag. This is one of the core tactics for surviving night shift nursing long-term.
On your first few shifts:
Tell your charge nurse or preceptor you are new to nights. Most experienced night shift nurses remember the adjustment and will look out for you. Nights have a different team culture than days, and building those relationships early makes a significant difference.
For a deeper look at building a sustainable nurse sleep schedule, including how to manage sleep across stretch days, read our dedicated guide.
How Do You Sleep Well After a Night Shift?
Sleep is the single most important variable for nurses surviving night shift nursing. Everything else, including alertness, decision-making, and emotional resilience, depends on it. A Scientific Reports study found that night shift ICU workers averaged only 5.74 hours of sleep between consecutive night shifts, well below the 7 to 9 hours needed for cognitive recovery.
Build a consistent sleep anchor. The CDC recommends that night nurses maintain a partial sleep schedule even on days off: go to bed around 3 to 4 AM and wake around noon or 1 PM. This keeps an overlapping window of sleep consistent every 24 hours rather than fully flipping your schedule and creating perpetual jet lag.
Your sleep environment checklist:
Use this checklist to determine if you are setting yourself up for success.
| Factor | Target |
|---|---|
| Light | Blackout curtains or sleep mask: complete darkness |
| Temperature | 65 to 68°F (18 to 20°C) |
| Noise | White noise machine or earplugs |
| Phone | Do Not Disturb mode, exception for emergency contacts only |
| Commute | Wear sunglasses on the drive home to limit morning light exposure |
| Post-shift meal | Light and low-glycemic to avoid digestive disruption during sleep |
Go straight to bed after your shift. Morning light is one of the most powerful circadian cues your body has. Every minute of sunlight exposure on your drive home signals “wake up” to your brain. Wearing sunglasses, even on a cloudy morning, reduces this signal significantly.
How Do You Stay Alert During the 3 AM Dip?
The 3 AM wall is not a myth or a mental block. It is a real physiological event. Your core body temperature hits its lowest point between 2 and 4 AM, and melatonin levels are typically at their peak, both of which combine to produce the strongest drive for sleep in the 24-hour cycle. Alertness scores in nursing research drop measurably during this window on every night shift, regardless of how much sleep a nurse got beforehand.
The goal during this window is not to fight it head-on. Work with it.
Strategic task management around the dip:
- Front-load your highest-acuity patient care and complex assessments before 2 AM when your cognitive performance is still near its peak.
- Use the 3 to 4 AM window for charting, documentation, restocking, and lower-complexity tasks that do not require rapid clinical judgment.
- Schedule any allowed break time during this window if patient census permits.
In-the-moment strategies that work:
1. Cold water on your face and wrists. A quick drop in skin temperature activates alerting mechanisms. It is temporary, but it buys 15 to 20 minutes of sharper focus.
2. Brief physical movement. Even five minutes of walking the unit or doing calf raises at the nurses station raises your heart rate enough to counter sleepiness. A review in Cureus (2025) found physical activity interventions consistently improved alertness in night shift healthcare workers.
3. Bright light exposure. The same Cureus review identified blue-enriched bright light as one of the most consistently effective interventions for maintaining alertness on night shifts. If your unit has lighting control, turn it up during this window.
4. Strategic caffeine. A small dose (40 to 60 mg, equivalent to half a cup of coffee) can bridge the dip, but only if you are 4 to 6 hours away from your planned sleep time. More on this in the caffeine section below.
What Should Nurses Eat During a 12-Hour Night Shift?
Your digestive system follows the same circadian rhythm as the rest of you. NIOSH guidelines recommend reducing food intake between midnight and 6 AM when possible, because your gut is biologically primed for rest, not digestion. Eating large meals during this window increases risk for gastrointestinal distress, blood sugar instability, and post-meal sleepiness, none of which you need at 3 AM.

The framework for a 12-hour shift:
The table below lays out an example eating plan for a 12-hour shift.
| Timing | What to Eat | What to Avoid |
|---|---|---|
| Pre-shift meal (1 to 2 hours before) | Lean protein + complex carbs + vegetables | Heavy, fried, or high-fat meals |
| Early shift snack (2 to 3 hours in) | Greek yogurt, nuts, hard-boiled eggs | Sugary snacks, energy drinks |
| Mid-shift meal (around hour 6) | Balanced bowl: protein + whole grain + veggies | High-glycemic carbs, fast food |
| Late shift snack (9 to 10 hours in) | Fruit, nut butter, whole grain crackers | Caffeine (if sleeping within 4 to 6 hrs) |
| Post-shift meal | Light: oatmeal, cottage cheese, banana | Large meals that slow sleep onset |
Meal prep is your highest-ROI habit. After a 12-hour shift, you will not make good food decisions. Prepare your shift meals on your days off. Batch cook proteins (grilled chicken, hard-boiled eggs, baked salmon), portion snacks in advance, and pack everything the night before. See our full night shift diet guide for specific meal ideas and weekly prep schedules.
How Should Nurses Manage Caffeine on Night Shift?
Caffeine is a tool, not a solution. Used correctly, it extends your alertness window without wrecking your post-shift sleep. Used incorrectly, it destroys sleep quality and creates a cycle where you need more caffeine to compensate for the poor sleep that caffeine caused.
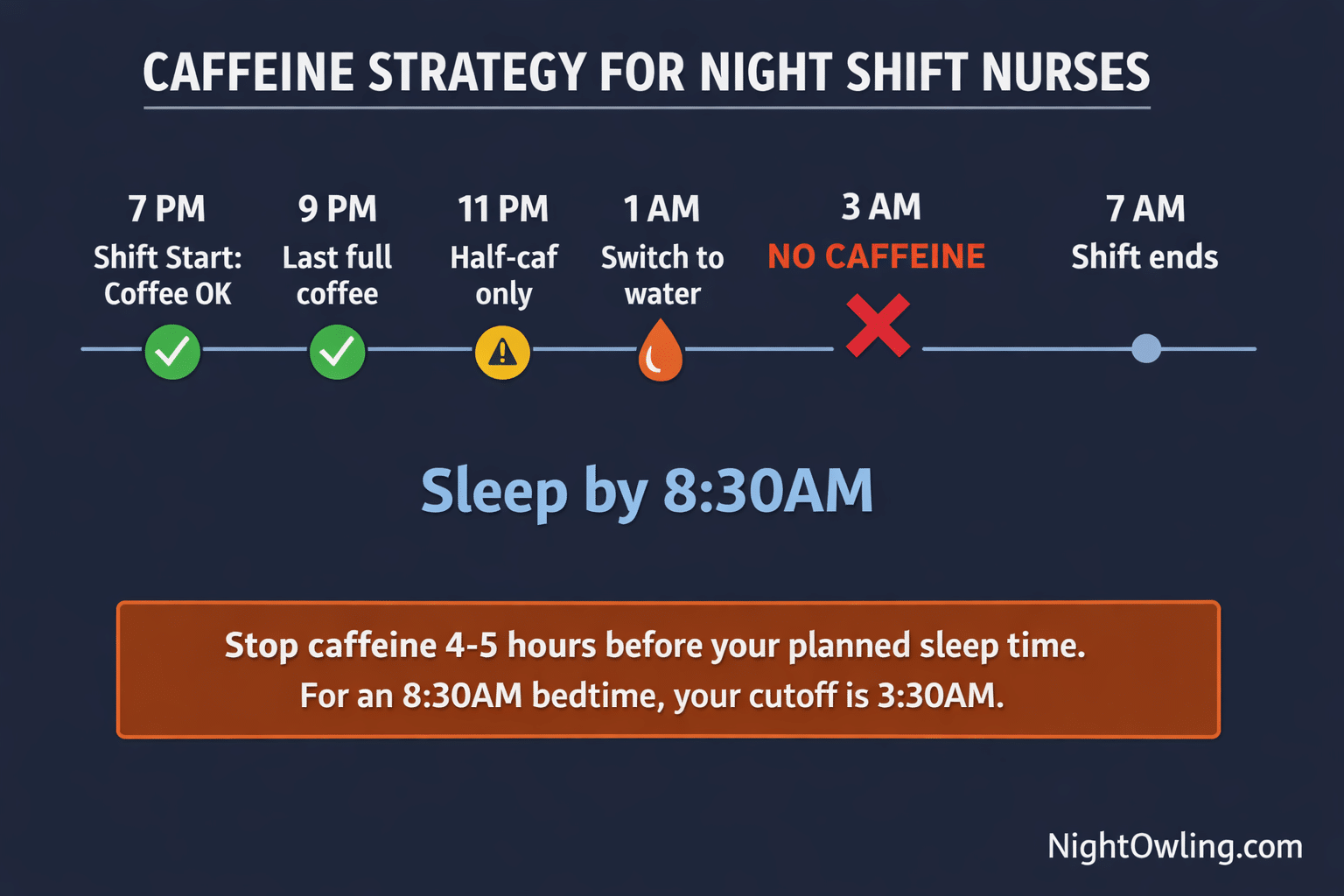
The core rule: Stop all caffeine 4 to 6 hours before you plan to sleep. A sleep medicine study found that caffeine taken six hours before bedtime still reduced total sleep time by more than one hour, even when subjects did not notice subjective sleep disruption.
Caffeine plan for a 7 PM to 7 AM shift (sleeping at 9 AM):
Below is an example caffeine plan for a 12 hour shift.
| Time | Dose | Purpose |
|---|---|---|
| 6 to 7 PM (pre-shift) | 100 to 150 mg | Primary alerting dose |
| 10 to 11 PM (optional) | 50 to 80 mg | Top-up if needed |
| After midnight | Avoid scheduled caffeine | Protect post-shift sleep |
| 2 to 3 AM only if necessary | 40 to 60 mg max | Bridge the dip only |
| 3 AM onward | None | Last caffeine must clear before 9 AM sleep |
Caffeine has a half-life of 4 to 6 hours. If you drink 200 mg at 4 AM and try to sleep at 8 AM, you still have roughly 100 mg active in your system. That coffee is not helping you recover. It is cutting your deep sleep in half.
- Daily limit: Stay under 400 mg per 24 hours. Most nurses hit this limit without realizing it across a full shift with multiple cups of coffee plus snacks.
How Do Night Shift Nurses Stay Connected Socially?
Social isolation is one of the most underreported costs of surviving night shift nursing. You miss dinners, weekends, and most of the events that structure a normal social life. Research in Health Promotion found that night shift nurses experience significantly higher rates of anxiety and depression than non-shift nurses, with social disconnection identified as a key contributing factor.
Practical strategies:
- Be explicit with your family and close friends about your schedule. Most scheduling conflicts come from a lack of visibility, not a lack of willingness. Share your shift calendar monthly.
- Identify your overlap windows. If you sleep from 8 AM to 3 PM, you have late afternoons free before your next shift. Those hours are more available for connection than you may realize.
- Build unit community. Night shift teams often develop a tighter culture than day shift because you rely on each other more. Invest in those relationships. Bring food to share, check in with your colleagues, and treat the team as a genuine support system.
- Use asynchronous communication strategically. Voice notes, scheduled texts, and shared family apps let you stay connected without requiring everyone to be awake at the same time.
The adjustment is real, and it takes time. Most night shift nurses report that it takes three to six months before the social rhythm starts to feel manageable. Building these social habits is part of how to survive night shift nursing for the long term.
When Is the Best Time for Night Shift Nurses to Exercise?
Exercise timing matters more for nurses surviving night shift nursing than for day workers because the wrong timing can interfere with your already-compressed sleep window. Getting this right is one of the underappreciated pillars of surviving night shift nursing sustainably.
Best options:
- Before your shift (late afternoon). A moderate workout 2 to 4 hours before your shift raises your core body temperature and heart rate, then lets them fall as you start work, which actually supports alertness early in the shift.
- After sleeping, before your next shift. If you have a stretch of nights, exercising after your recovery sleep gives you the physical and mental reset without cutting into sleep time.
Avoid intense exercise within 2 hours of sleeping. Post-exercise cortisol and elevated heart rate delay sleep onset. After a 12-hour shift, your goal is to transition to sleep as efficiently as possible.
Moderate exercise 3 to 5 times per week consistently shows benefits for night shift workers: better daytime sleep quality, reduced fatigue on shift, and lower rates of the metabolic issues associated with long-term night work. Keep sessions to 30 to 45 minutes if time is tight. Consistency matters far more than intensity.
When Should a Night Shift Nurse Ask for Help?
Night shift nursing fatigue is cumulative. It builds over weeks and months in ways that are hard to self-assess, because the cognitive impairment that comes with sleep deprivation also impairs your ability to recognize that impairment.
Signs you need to escalate or seek support:
- You are making documentation errors or near-miss medication mistakes more frequently
- You feel emotionally detached from patients. Not just tired, but flat.
- Your sleep is not recovering between shifts even when you have adequate time
- You are using caffeine or alcohol to manage the shift cycle rather than as occasional tools
- Colleagues have mentioned concern about your wellbeing or performance
Talk to your charge nurse, nurse manager, or employee assistance program early. Night shift nursing has real, documented health risks over time. A JAMA cohort study found that ten or more years of rotating night shift work was associated with a 20% decrease in the odds of healthy aging. These are not scare statistics. They are the reason early intervention and sustainable habits matter.
For a full overview of how to survive night shift nursing over the long term, including health and career considerations, read our night shift nursing guide.
If you are looking for personalized support and strategies for working night shifts, explore our individual resources.
FAQs: How to Survive Night Shift Nursing
How long does it take to adjust to night shift nursing?
Most nurses report noticeable improvement within two to four weeks. Full circadian adaptation, if it occurs at all, can take several months. The adjustment is faster when you cluster shifts, maintain a consistent sleep schedule on days off, and follow structured sleep hygiene practices.
How many hours of sleep should a night shift nurse get?
The same as anyone else: 7 to 9 hours per 24-hour period. The challenge is that daytime sleep is physiologically harder to sustain because daylight and social noise work against it. Blackout curtains, white noise, and a consistent sleep window significantly improve daytime sleep quality and duration.
Is it normal to feel sick during the first weeks of night shift?
Yes. Gastrointestinal symptoms, headaches, and general malaise during the first week or two are common and reflect the disruption to your circadian rhythm. These typically improve as your body adapts. If symptoms persist beyond three to four weeks or are severe, consult your primary care provider.
Can you stay healthy long-term as a night shift nurse?
Yes, with deliberate management. Long-term rotating night shift work carries documented health risks, but nurses who consistently prioritize sleep, exercise, and nutrition show significantly better outcomes. Many nurses work nights for decades without major health consequences. The key is treating your health habits as non-negotiable, not optional.
What is the hardest part of surviving night shift nursing for most nurses?
Most nurses report that the social and family schedule disruption is harder to manage long-term than the physical fatigue. Building explicit communication systems with the people in your life, and finding a community within your night shift team, are the highest-leverage social strategies.
Looking for more guidance on thriving as a night shift worker? Browse the NightOwling blog or explore tools and support built for individuals at NightOwling for Individuals.


